
Helping parents of neurodivergent children reduce mealtime stress and expand food variety.
Helping neurodivergent children with autism, ADHD, and restrictive eating feel confident around food by supporting parents with practical, dietitian-led feeding guidance.
If mealtimes are filled with anxiety, sensory overwhelm, or nutrition worries, you are not alone. I help families to feel confident feeding their child.
If you are looking for simple steps that make a real difference, this is where to begin.
I went from feeling helpless watching meals go untouched to creating mealtimes where kids explore food willingly.
kristy jordan
dietitian & feeding therapist
Hi, I'm Kristy!
I know how exhausting and disheartening mealtimes can feel, especially when your child is autistic and food feels like a daily battle. I’ve seen the stress, the worry, and the frustration when every strategy seems to fall short.
Through years of working alongside families as a feeding therapist, I’ve learned how to create a mealtime environment that encourages eating. My approach helps children feel safe exploring food at their own pace, while giving parents the tools and confidence to support them without pressure.
I’ve walked with many families of autistic children as they’ve rebuilt trust at the table, celebrated progress, and rediscovered joy in mealtimes - and I’d love to help you do the same.

Support your child’s health and development by making achievable progress with food today

Are you worried about your child's nutrition?
A free, printable workbook for parents
How many times have you wanted to feel confident about your child’s nutrition, but felt stuck between worrying too much and avoiding thinking about it altogether?
If your child eats a limited range of foods, it is natural to wonder whether they are getting what they need.
This Nutrition Check-In is designed to help you understand where your child’s intake may already be okay, and where extra support might be helpful.
Ready to build the family meals of your dreams?

Join The Community
Get guidance from experts and join a supportive community of parents who understand. Together, we’ll help you create a mealtime environment where your child's needs are being met, and you can relax knowing you are doing everything you can to support them in their journey.

Follow Me On Instagram
Get daily tips, inspiration, and behind-the-scenes insights to help you stay motivated and improve your relationship with your child at mealtimes.

Subscribe To The Newsletter
Subscribe to the Grate Adventure newsletter for actionable strategies, expert advice, and inspiring stories to help you to learn what changes you can make to help your child, starting today.
Ready to build the life of your dreams?

Let's chat
Ready to work with a coach to uplevel your life and business?
Listen to the
Podcast
view my
services
read the
BLOG
Let's chat
Ready to work with a coach to uplevel your life and business?


Let's learn
Learn at your own pace and make quantum leaps.
Student Love Notes
We've helped so many incredible students to find success as Virtual Assistants...

The VA Business Blueprint helped me to go from feeling completely stuck to starting my business and getting my first client!
Ellen, business name

I enrolled in the VA Services Academy feeling completely lost - within 2 weeks I knew exactly what to offer & what to charge.
Ellen, business name

Beginner to Booked Out was a game-changer for me. Anna and her team are incredible and I'm booked out for the next 3 months!
Ellen, business name
New on the blog...

What Is Feeding Therapy? (And Why It's Probably Not What You Think)
If you've typed "feeding therapy" into Google at 11pm while your child refused dinner for the third night in a row - first of all, you're not alone. Second, you've probably come away more confused than when you started.
Feeding therapy. It sounds clinical. Maybe even a little scary. You might be picturing a sterile room, a therapist in a white coat, and your child being made to touch, smell, or eat foods they're terrified of. Maybe you've imagined tears, bribery, sticker charts, or someone literally putting food in your child's mouth.
Here's the truth: that's not what good feeding therapy looks like. And it's definitely not what it should look like.
Let's break it all down - what feeding therapy actually is, where it came from, and what a modern, child-centred approach really means for your family.
Part 1: So... What IS Feeding Therapy? (Spoiler: Nobody Fully Agrees)
Here's something that might surprise you: there is no single, universally accepted definition of "feeding therapy."
Seriously. The professionals who deliver it - Speech-Language Pathologists, Occupational Therapists, Dietitians, Psychologists - all define it slightly differently based on their training and lens.
What the field does broadly agree on is this:
"Feeding therapy is a specialised, multidisciplinary intervention aimed at helping individuals - most often children - eat and drink safely, comfortably, and efficiently."
(General clinical consensus, PubMed & pediatric feeding literature)
In 2019, advocates including the organisation Feeding Matters worked to create a unified diagnosis called Pediatric Feeding Disorder (PFD), defined as:
"Impaired oral intake that is not age-appropriate, lasting more than two weeks, with dysfunction in one or more domains: medical, nutritional, feeding skills, or psychosocial."
(PFD Consensus Definition, 2019 — Feeding Matters)
This was a huge step forward. But even with a clearer diagnosis, the treatment - feeding therapy itself - still looks wildly different depending on who you see.
Some of the most well-known approaches include:
SOS (Sequential Oral Sensory) Approach - A play-based approach where children explore food through touch, smell, and taste at their own pace, without pressure. (SOS Approach to Feeding)
Responsive Feeding Therapy (RFT) — Defined as "an overarching approach to feeding and eating interventions applicable to multiple disciplines and across the lifespan. RFT facilitates the (re)discovery of internal cues, curiosity, and motivation, while building skills and confidence. It is flexible, prioritises the feeding relationship, and respects and develops autonomy." (Rowell, Wong, Cormack, Moreland et al., Responsive Feeding Therapy White Paper, Version 2, 2023 - responsivefeedingpro.com)
Behavioral/ABA-informed approaches - Use positive reinforcement and structured exposure to reduce food refusal and expand diet. (Applied Behavior Analysis literature)
The bottom line? Feeding therapy is an umbrella term. What it looks like depends entirely on the approach - and not all approaches are created equal.
Part 2: A (Surprisingly Wild) History of Feeding Therapy
To understand where feeding therapy is today, it helps to know where it came from. Buckle up - some of this will make your jaw drop.
The Early Days: "Just Eat It" (Pre-1980s)
For most of history, children who struggled to eat were simply told to eat. "Clean your plate." "You'll eat when you're hungry enough." "There are starving children who would love that food." Sound familiar?
Feeding difficulties were seen as a parenting problem, a discipline problem, or just a phase. There was no specialised support - just pressure, and plenty of it.
The Behavioural Era: Compliance at All Costs (1980s–2000s)
As feeding therapy emerged as a specialised field within Speech-Language Pathology and Occupational Therapy, the dominant approach was heavily behavioural. The thinking was: eating is a behaviour, so we can shape it.
This led to techniques like:
Escape extinction (also called "non-removal of the spoon") - a child was required to accept a bite of food before being allowed to leave the table or end the meal. Refusal was simply not an option.
Mandibular pressure - physically opening a child's jaw to place food in their mouth.
Hunger-based tube weaning - withholding tube feeds to make a child hungry enough to eat orally.
Force feeding - physical pressure to eat, sometimes with restraint.
Did these approaches "work" in the short term? Sometimes, in the narrowest sense - a child might eat more bites. But at what cost? Anxiety, trauma, a destroyed relationship with food, and a child who learned that mealtimes were a battleground. For neurodivergent children, children with sensory differences, or children with anxiety - these approaches could cause lasting harm.
The Shift: From Compliance to Connection (2010s–Now)
The current era of feeding therapy is characterised by a fundamental rethink.
Key shifts include:
Moving away from force and pressure toward low-stress, child-led exploration
Recognising sensory and neurological differences as real, valid reasons a child struggles - not "bad behaviour"
Centring the parent-child relationship as the foundation of progress
Focusing on quality of life - happy mealtimes matter more than the number of bites taken
The rise of Responsive Feeding Therapy, which prioritises autonomy, intrinsic motivation, and the whole child
The field still has a long way to go - but the direction is clear. The best feeding therapy today looks nothing like it did 30 years ago.
Part 3: How the Grate Adventures Approach Is Different
So where does Grate Adventures fit into all of this?
Whether you've tried feeding therapy before or you're completely new to it, here's what I want you to know: my approach is built on one core belief - your child does not need to be fixed.
While there may have initially been a problem that started your child's struggle with food, it is the environment, the pressure, the mealtime dynamics, and the lack of the right kind of support that can cause feeding issues to continue. When we change those things, children change - not because we made them, but because they wanted to.
Here's what that looks like in practice:
I will never pressure your child to do anything. Not to touch a food, smell it, taste it, or even look at it. Instead, I focus on sparking intrinsic motivation - that natural, internal drive that makes a child want to explore. (This is such a powerful concept that I'm dedicating an upcoming webinar to it - more on that below!)
I modify the food, the environment, and the routine - not the child. Think deconstructed meals, food chaining (building from foods your child already loves), sensory-friendly environments, peer influence, and getting kids involved in food preparation. When a child helps grate the cheese, they're already halfway to trying it.
I use Division of Responsibility. Parents decide what, when, and where food is offered. Children decide whether and how much they eat. This simple shift removes an enormous amount of pressure from mealtimes - for everyone.
I draw on CBT-AR principles to gently address the anxiety and thought patterns that can make food feel genuinely frightening for some children.
And everything I do is guided by my framework The Path:
Trust: Remove pressure, establish clear feeding roles, rebuild the parent-child relationship
Opportunity: Create a sensory-friendly environment and structured, pressure-free opportunities to explore food
Growth: Build skills and confidence through food chaining, cooking involvement, and activities within your child's comfort zone
Independence: Support your child to set their own food goals, navigate real-world eating, and advocate for their own needs
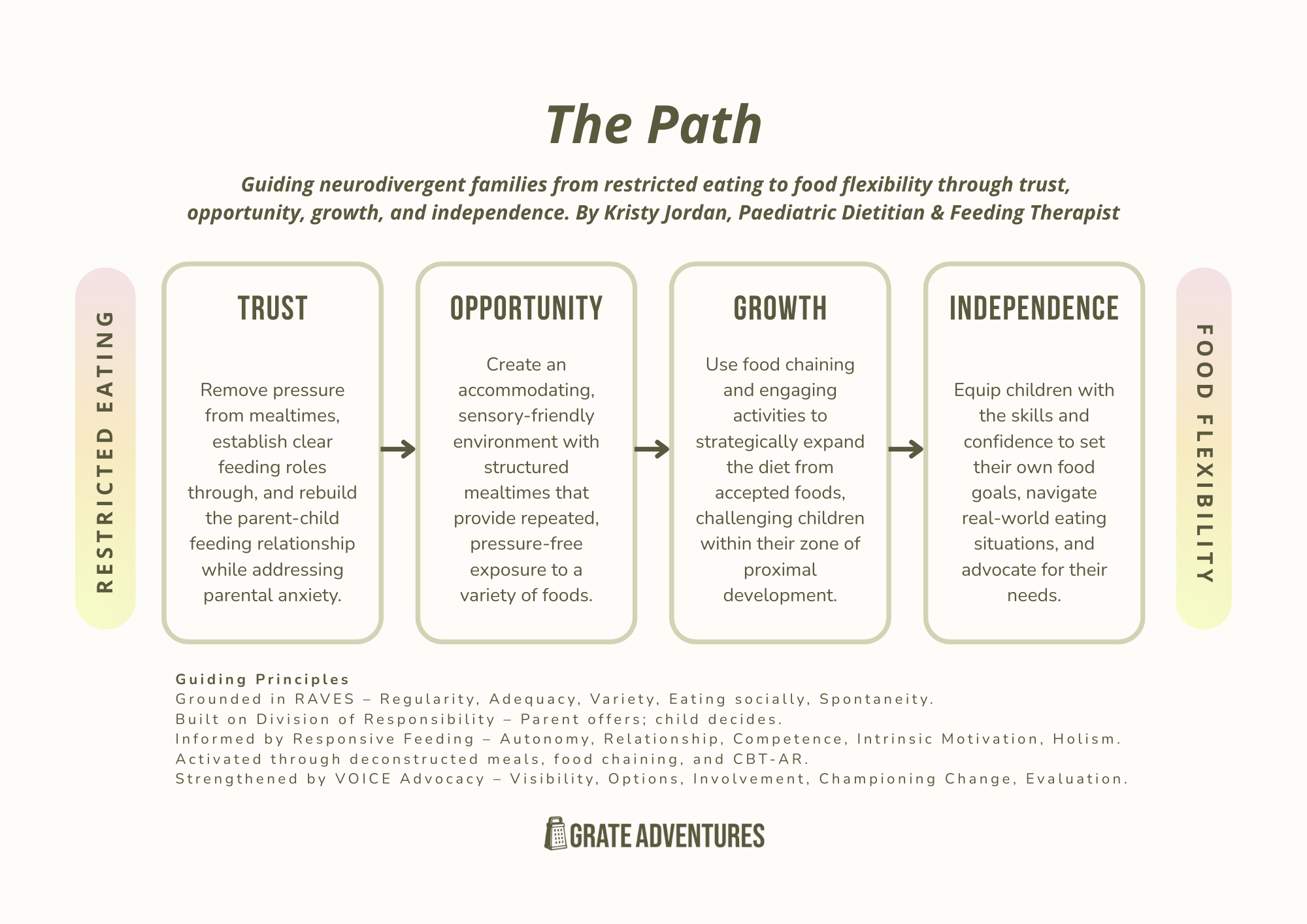
The outcome families experience isn't just "my child eats more foods" (though that does happen - every single client I've worked with has tried new foods). It's a happier relationship with food and eating - for the whole family.
Part 4: What Is Feeding Therapy at Grate Adventures?
Here's my definition - written specifically for the families I work with:
Grate Adventures Feeding Therapy is a responsive, child-centred approach that supports children and families to build a happier, more flexible relationship with food - without pressure, force, or fear.
Rather than trying to change the child, we focus on three things: modifying the food (making it more approachable), modifying the environment (making mealtimes feel safe and enjoyable), and involving children in food preparation and mealtime routines (so they become curious, confident participants rather than reluctant bystanders).
Grounded in Responsive Feeding Therapy, the Division of Responsibility, food chaining, and CBT-AR principles, the Grate Adventures approach honours each child's unique sensory profile, pace, and intrinsic motivation. Progress isn't measured in bites - it's measured in confidence, curiosity, and connection.
Ready to Start the Adventure?
If this resonates with you - if you're tired of stressful mealtimes, tired of feeling like you're failing, and ready for a different way - I'd love to have you join us.
The Grate Adventures Feeding Therapy Community is a membership for families just like yours. Inside, you'll find:
The Path course content
A warm, supportive community of parents on the same journey
Live Q&A sessions with me
Challenges, tools, and resources to use at home - today
And coming very soon: a free webinar on intrinsic motivation — one of the most powerful tools you have as a parent. You won't want to miss it.
👉 Join Our Mailing List & Save Your Spot
Be the first to know when the membership opens, get early access, and never miss a free resource or webinar.
Sources: Feeding Matters & PFD Consensus Definition (2019); Rowell, Wong, Cormack, Moreland et al., Responsive Feeding Therapy White Paper v2 (2023), responsivefeedingpro.com; SOS Approach to Feeding; ABA feeding literature; Late 20th Century feeding therapy history via PMC & ASHA publications.

